It’s the time of year where we might start to neglect our bodies. Resolutions from the New Year have well and truly worn off, the Easter chocolate wrappers have amassed and the cooler weather is making a stroll in the park much less enticing.
The news is also deeply depressing and new disasters are churning out everyday. Because there are currently no ‘dull global news days’, it means new and interesting research is being plonked in the backseat.
Let’s give some of it the limelight it deserves. Today, we’re looking at health research.
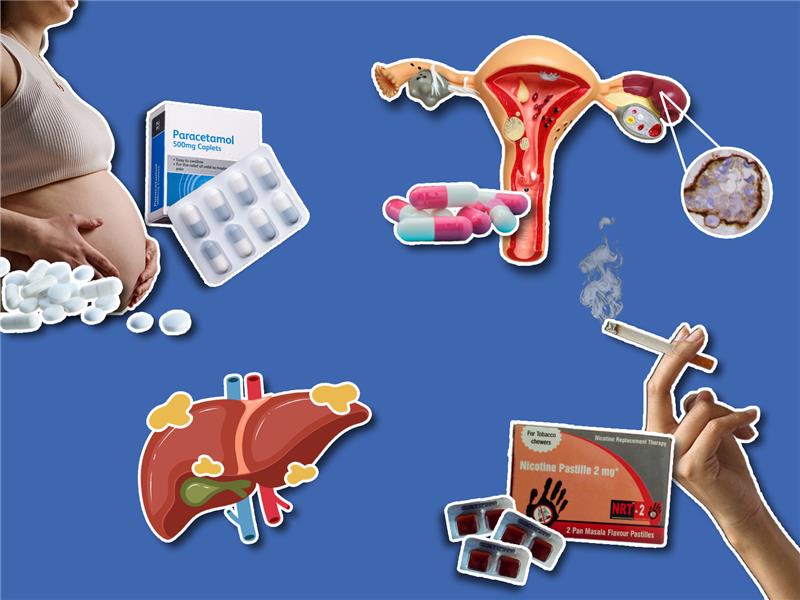
No, paracetamol still doesn’t cause autism
It was Donald Trump and his team who suggested last year that taking paracetamol during pregnancy can cause autism in the unborn foetus.
Since then, many studies have sought to disprove this, including a new paper from Denmark.
The study found that taking paracetamol whilst pregnant does not lead to an increased risk of autism.
Researchers analysed data from over 1.5 million children born in Denmark over 25 years, including 31,000 children who were exposed to paracetamol before they were born.
They found that of the 31,000 children who were exposed to paracetamol, 1.8% of them went on to be diagnosed with autism. The remaining 1.47 million children had an autism diagnosis rate of 3%.
Don’t get liver-ed with me
From good news, to some not so good news – a new study suggests that 1.8 billion people could have liver disease by 2050.
Non-alcoholic fatty liver disease is associated with obesity, high blood pressure and type 2 diabetes. It’s estimated that 1.3 billion people suffered from liver disease in 2023 – a 143% increase since 1990.
The extra half a billion suffers are expected to be driven by a growing population with growing levels of obesity and more sedentary lifestyles.
Reading that makes me want to blast James Brown’s ‘Get Up Offa That Thing’ and leap out of my chair.
I sat back down after reading that despite higher rates of the disease, the impact on people’s health has remained stable. This is likely due to advancements in medical treatment.
Researchers suggest recognising liver disease as a global health priority and giving the disease an awareness (aka marketing) campaign.
Smoking is bad for you! And expensive to quit…
Apparently telling people smoking is bad for them isn’t enough to stop them smoking. A new editorial in Public Health Research & Practise wrote that the Australian Federal Government is not doing enough to help people quit tobacco.
The authors find that while smoking has declined, “rates remain much higher among disadvantaged populations”.
Nicotine replacement therapy (NRT) can cost around $200 a month. For opioid treatment, monthly costs are around $7.70 with government subsidies.
The authors are calling to have similar levels of governmental support and funding for those trying to quit tobacco.
Potential new ovarian cancer treatments
Back to some good news! Two drug trials have found potential new treatments for platinum-resistant ovarian cancer.
That is, a cancer that returns within six months of platinum-based chemotherapy. This type of cancer generally has a very poor prognosis.
However, two new trials are providing hope for patients.
The ROSELLA trial tested relacorilant, a medication used in the treatment of Cushing’s syndrome, alongside their usual cancer treatment. Those in the trial reduced their risk of death by 35% and on average, lived four months longer than patients not taking relacorilant.
The second trial tested an antibody-based treatment used in other cancers. Patients in the trial reduced their risk of death by 18%.
Stem cells and HIV remission
The final piece of health news is small but mighty. In 2006, a male patient was diagnosed with HIV. His sibling had a mutation in their stem cells to treat a blood cancer variant (CCR5Δ32/Δ32 if you’re interested), and in 2020, the HIV-positive patient received a stem cell transplant.
Since the transplant, the donor stem cells were found to be replacing the patient’s immune cells.
Researchers examined over 65 million of the man’s cells and detected “no virus capable of multiplying” and found that his “HIV antibody levels declined over four years after transplantation”. The man has been declared to be in long-term HIV remission.
Whilst this has only been tested in one patient, it provides hope for those living with HIV – as long as they have a sibling with a useful stem cell mutation.